Fields of interest
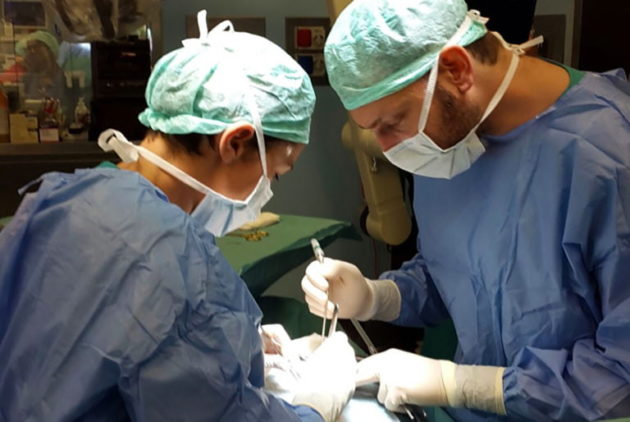
Neuroncology and surgery of central nervous system tumors (brain and spinal cord)
Central nervous system tumors are pathologies with a significant functional impact on patients' lives. They are neoplasms affecting the brain and the spinal cord. This category includes gliomas (e.g., astrocytomas, glioblastomas, oligodendrogliomas, ependymomas), meningiomas, neuromas, adenomas, metastases, and other rarer nosological entities.
To date, the therapeutic strategy involves multidisciplinary collaboration between different professional figures: neurosurgeons, neuro-oncologists, radiation oncologists, and researchers. It is essential that patients affected by central nervous system tumors are treated in reference centers, equipped with all these professionals and the most modern technologies in the field. For successful treatment, therapy must be individualized to each individual case, according to the most current scientific evidence on the subject.
I have been always involved in preclinical cancer stem cell research, actively participating in trial protocols for new drugs and gene therapy in the field of brain tumors. I am one of the coordinators in the multidisciplinary neuro-oncology team (disease unit) at San Raffaele Hospital. As neurosurgeon, I specialized in brain and skull base tumor surgery, applying the best technologies currently available to my daily clinical practice, such as endoscopy, intraoperative fluorescence and ultrasound, confocal microscopy of resection margins, neuronavigation, and neurophysiological stimulation (as in awake surgery).
I have published numerous scientific articles in specialized journals and two books on surgical techniques, which have been worldwide distributed, which are the result of my many years of clinical and scientific work in this field.
Surgery of degenerative and traumatic spinal pathology
Degenerative spinal disease is highly prevalent in the general population; it is the leading cause of absenteeism in industrialized countries and significantly impacts patients' quality of life and functional prognosis. It refers to a heterogeneous group of conditions, including disc pathologies (e.g., herniated discs, protrusions, and disc defects), stenosis (e.g., spinal canal, foraminal, and recess stenosis), instabilities (spondylolisthesis, spondylolysis), and secondary deformities (scoliosis and degenerative kyphosis).
The treatment of patients with these conditions is extremely complex, beginning from therapy indications till to proper selection of patient and surgical technique.
The technological development has completely revolutionized the therapeutic approach to spinal pathology. Minimally invasive surgical techniques have played a key role, significantly reducing the impact of surgery on patients, optimizing clinical and functional outcomes and reducing operating times and hospital stay.
As neurosurgeon, I have developed my expertise in minimally invasive surgical techniques, from surgery for hernia and stenosis using small tubular retractors to more complex minimally invasive arthrodesis techniques with anterior, lateral, and posterior approaches.
Reducing the impact of surgery on patients has allowed me to optimize clinical and functional outcomes, improving both short- and long-term quality of life.
Surgery of spine tumors
Spinal tumors are neoplasms developing from the vertebrae and tend to spread and infiltrate surrounding tissues and organs.
The most common are secondary tumors (metastases) and tumors originating from bone marrow disorders (myelomas, plasmacytomas). Primary vertebral tumors (chordomas, sarcomas, osteomas, chondromas, aggressive angiomas) are extremely rare.
As is easy to understand, the extreme heterogeneity of these pathologies requires careful diagnostic assessment to guide the best treatment choice for each individual patient.
To date, the strategy necessarily requires multidisciplinary collaboration between different professionals: neurosurgeons, oncologists, and radiation oncologists. As with brain tumors, it is essential that patients are treated in reference centers equipped with these professionals and the most modern technologies.
As neurosurgeon, I have extensively studied spinal tumors and the development of minimally invasive techniques for treating vertebral tumors, publishing articles on surgical techniques in this field. The use of intraoperative stimulation and monitoring, spinal navigation, and advanced imaging techniques, combined with collaboration with thoracic, general, and vascular surgeons, has enabled previously unimaginable advances in the management of these conditions, substantially reducing morbidity and complication rates.
The multimodal approach combined with the development of therapeutic pathways based on the latest scientific evidence has also significantly improved oncological outcomes and disease control.
Stereotactic radiosurgery
Radiosurgery is a relatively recent technology that involves the use of high-intensity radiation focused on a target (collimation principle), where it exerts its therapeutic effect while protecting surrounding healthy tissue. One of the most widely used technologies in this field is stereotactic radiosurgery with Gamma Knife.
Gamma radiation treatment is indicated for numerous pathologies: intracranial tumors (metastases, meningiomas, neuromas, adenomas), vascular malformations (cavernomas, vascular malformations, arteriovenous fistulas), pain management (trigeminal neuralgia), and functional and psychiatric disorders (e.g., tremor, obsessive-compulsive disorder). The application of this technology has revolutionized patient care, allowing to treat conditions that once required demolitive approaches with a non-invasive method, mostly in outpatient settings.
A thorough understanding of radiobiological principles is essential for proper patient selection and the correct indication for treatment.
Reference centers equipped with this technology allow to expand the therapeutic offering to patients, in the perspective of individualized medicine with low functional impact.
A multidisciplinary team composed of a neurosurgeon, radiation oncologist, and medical physicist discusses each case and agrees on a shared treatment strategy.
I have always dedicated my clinical and scientific interest to this technology, contributing to its development through numerous scientific articles in specialized journals.
Surgery of central nervous system vascular pathologies (brain and spinal cord)
Vascular disorders of the brain and spinal cord are an extremely heterogeneous class of conditions, all of which share a common origin: a congenital defect in the development of the vascular tree. These include cerebral aneurysms (focal dilation of an intracranial arterial vessel), arteriovenous malformations (direct shunts between the arterial and venous systems in the absence of an intervening capillary bed), cavernomas/cavernous angiomas (low-flow communicating vascular gaps), and dural arteriovenous fistulas (direct connections between a vein and an artery bridging the meninges and brain parenchyma, often the result of previous trauma).
A common thread is their structural fragility, which leads to a risk of rupture of the malformation and subsequent bleeding. Each of them has a specific bleeding risk, which is however strongly influenced by the size and structural characteristics of the malformation.
An accurate diagnostic assessment, defining patient's individual bleeding risk, is therefore essential in order to establish the most appropriate therapeutic approach. This diagnostic process is now shared by neurosurgeons and interventional neuroradiologists. It is therefore essential that patients are treated in reference center that have both these professionals.
In recent years, endovascular techniques have revolutionized the treatment of these conditions with the ability to exclude the malformation from circulation, effectively eliminating the risk of bleeding, through the use of microcatheters inserted into peripheral arteries. This has ultimately made it possible to treat with minimally invasive techniques conditions that once required lengthy procedures and were burdened with the risk of significant complications.
As neurosurgeon, I have developed my expertise in the multimodal approach to vascular conditions, using, when indicated, surgery or radiosurgery, and collaborating with the team of interventional neuroradiologists to share recommendations in the most complex cases.
Surgery of peripheral nervous system tumors
The peripheral nervous system is the set of nerves that functionally connect the spinal cord to the rest of the body in a bidirectional fashion (afferent and efferent components, in other words, sensory and motor functions). At the cervical and lumbar levels, near the spinal column, the peripheral nerves are organized into structures called brachial and lumbar plexus, respectively, characterized by complex interconnections between nerve pathways (anastomoses). Considering that the peripheral nerve travels along anatomical corridors through muscles, vessels, and tendons (in the limbs) and in close proximity to deep organs in the visceral cavities, it is easy to understand the surgeon's need for a thorough knowledge of general anatomy.
The most complex cases require the combined expertise of multidisciplinary teams, including neurosurgeons, thoracic surgeons, general surgeons, and vascular surgeons. A constant in peripheral nervous system surgery is the use of intraoperative monitoring to minimize the risk of functional nerve damage during tumor dissection. Collaboration between neurosurgeons and neurophysiologists is therefore essential to the success of the procedure. Here too, accessing a reference center equipped with all these technologies and dedicated specialists is crucial.
Developing a qualification in peripheral nervous system oncology surgery requires specific training in anatomy and microsurgical technique. During my training, I spent long periods abroad in dissection laboratories to develop in-depth knowledge of the subject. My expertise in minimally invasive spinal surgery and the clinical-translational approach to neuro-oncology have also allowed me to develop specific expertise in the field.
Request an appointment
Dr. Gagliardi sees patients at his clinics in Milan, Bolzano, Bergamo and Como.

